CHANGING THE WAY WOMEN AGE.
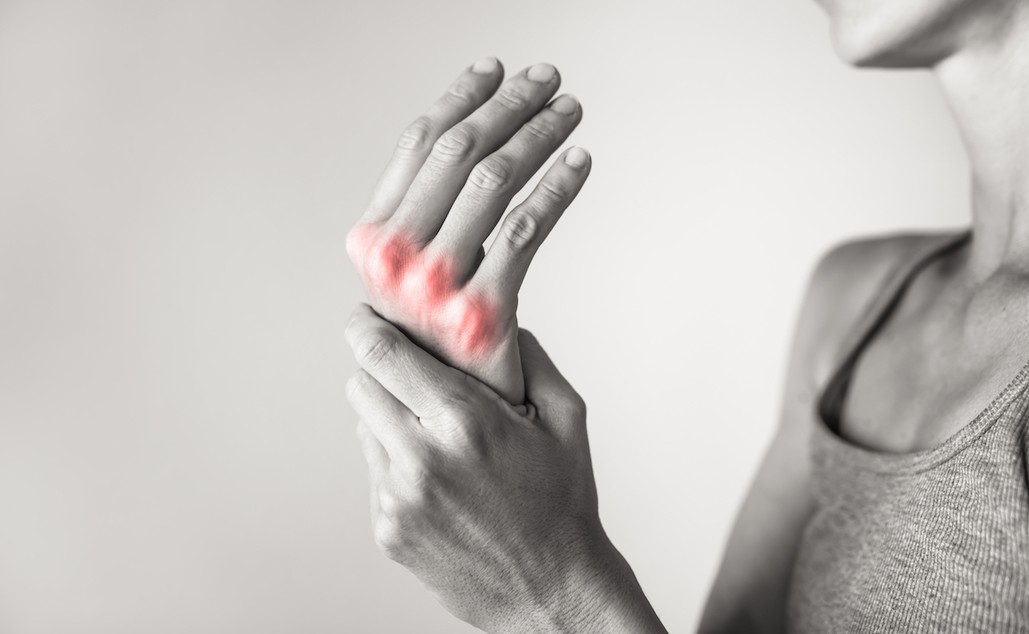
Inflammation Explained: Causes, Symptoms, and Treatment
Whether you like it or not, inflammation is a necessary pain you need to bear to keep your body healthy and functional.
Yes, inflammation affects your day-to-day life. It’s painful, affects your sleep, and limits your physical activities for days or weeks. It can even make you age faster!
But it’s important to understand that inflammation is one of your body’s defense mechanisms. It only becomes dangerous when it lingers longer than it should.
However, don’t be too quick to pop a pill to get rid of inflammation. There are other ways of reducing inflammation naturally.
Let’s discuss what inflammation is, its causes and symptoms, when it becomes threatening to your health, and how you can get rid of it naturally before it worsens.
What is inflammation in the body?
Inflammation is a defense and recovery mechanism that helps our body identify and remove harmful stimuli and heal itself. It’s a necessary adaptive immune system response to tissue damage, infection, and disease-causing microorganisms.
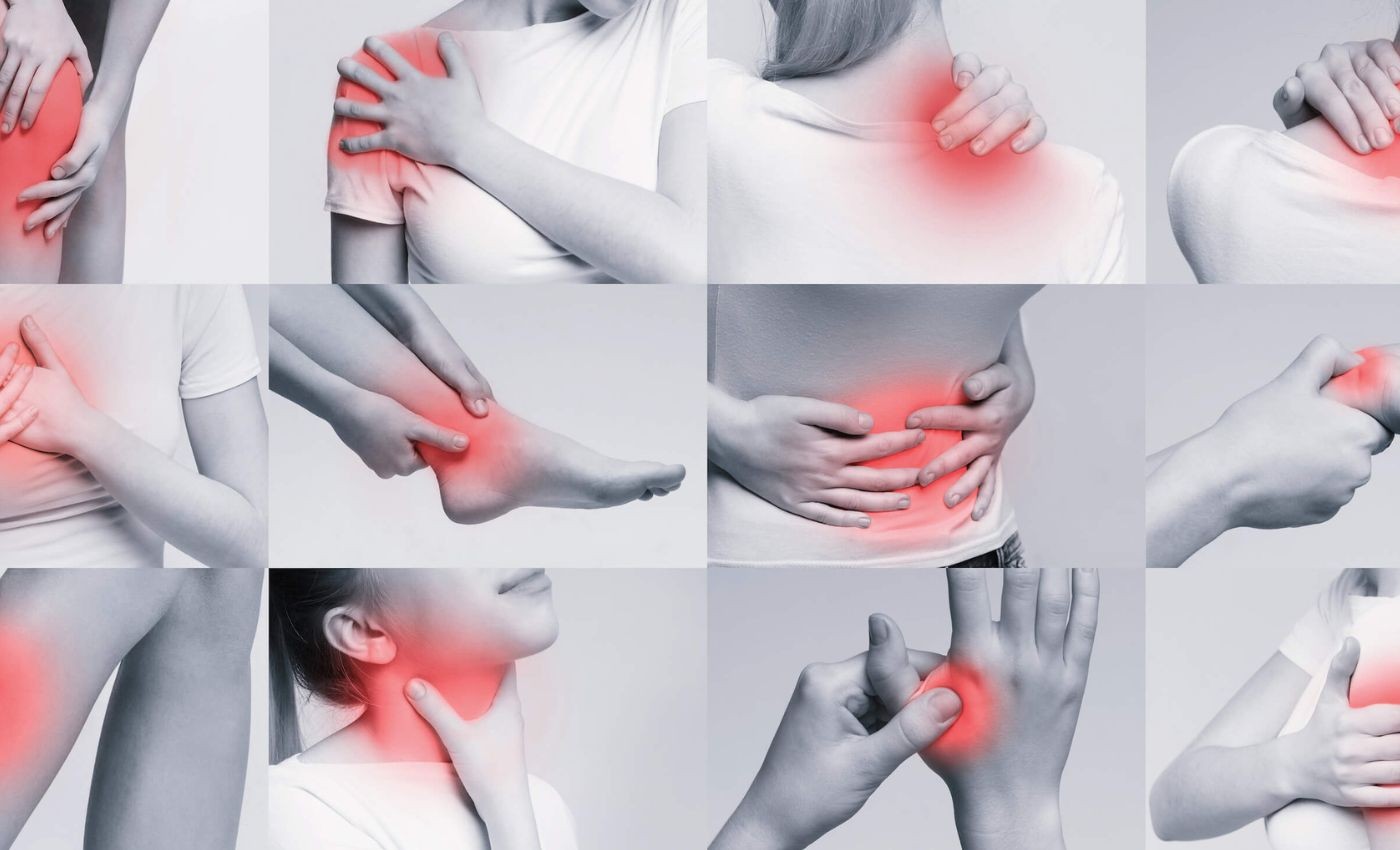
It involves communication and coordination among various cells and blood vessels to protect and heal the affected tissues in your body. The chemicals secreted by these cells result in redness, swelling, pain, fever, and other symptoms of inflammation.
However, this doesn’t mean that your immune system waits for damage to occur before it takes action. Instead, the inflammation process starts as soon as harmful microbes are detected to prevent them from harming the body.
Inflammation can occur in any organ in your body (e.g., your heart, lungs, liver, and kidneys), but it happens more often in the skin and the tissue underneath.
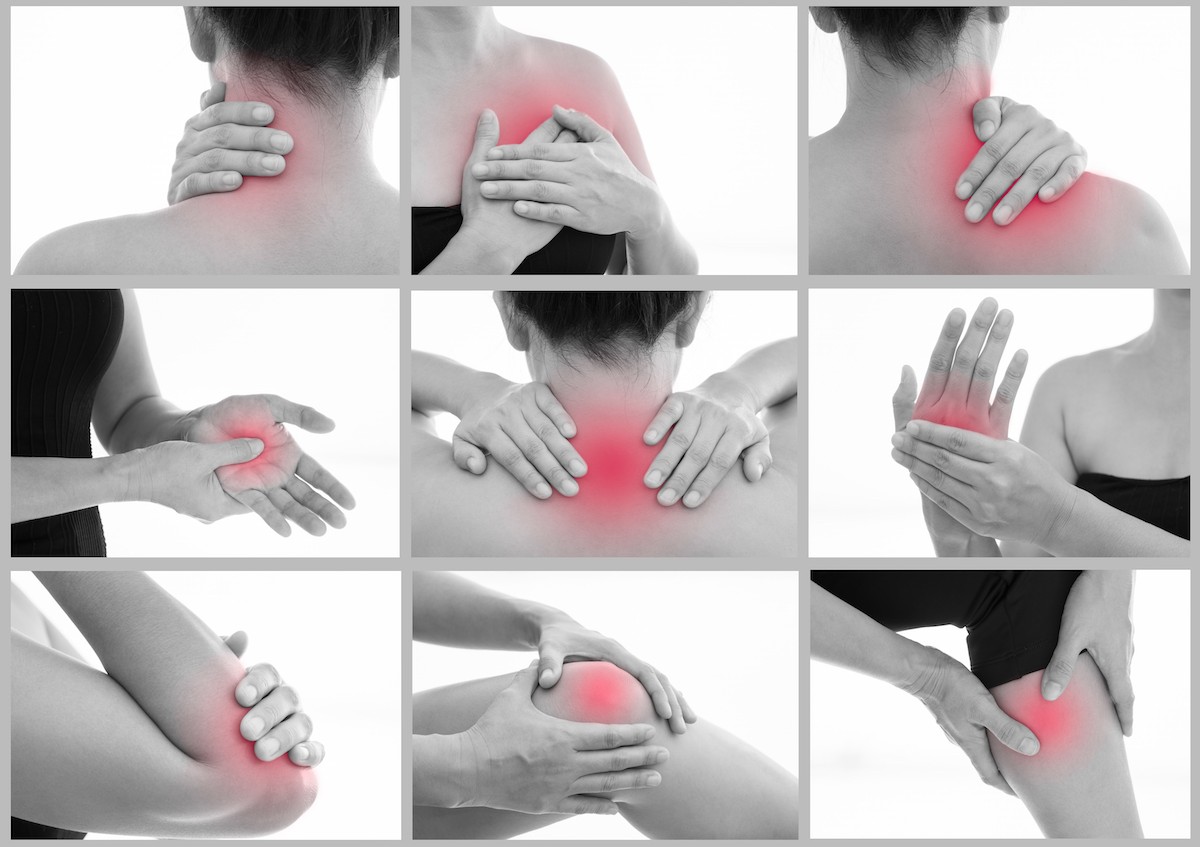
What causes inflammation, and what are its effects?
The Stages, Signs, and Symptoms of Inflammation
Many factors cause inflammation, but they can be broadly categorized as biological (bacteria, viruses, allergies), chemical (toxins, poisons), and physical (burn, frostbite, injuries to muscle and other tissue).
Inflammation occurs in three stages:
Inflammatory Response Stage
The inflammatory response starts when the immune cells or white blood cells (WBCs) detect a harmful stimulus (e.g., bacteria, viruses, toxins, etc.) or an injured cell or tissue.
This detection triggers the production of cytokines and other inflammatory chemicals. These chemicals widen the blood vessels to increase blood flow and make them more porous to allow more immune cells/WBCs and plasma fluid into the inflamed tissue.
The widening or dilation of the blood vessels (or vasodilation) and the surge of fluids cause redness, heat, swelling, and even pain.
Three things happen when the plasma fluid and WBCs work on the inflamed site:
1. The plasma fluid oozes into the site and delivers antimicrobial agents, platelets, and blood clotting agents to prevent the microbes from affecting other areas and stop the bleeding (if there are any).
2. Neutrophils, a type of WBC, come in and kill off bacteria. They also release chemicals called reactive oxygen species or ROS (a buildup of which causes oxidative stress) that can quickly eliminate pathogens.
3. Then, monocytes (another type of WBC) remove the dead pathogens, damaged cells, and dying neutrophils that fought bravely against the pathogens.
After the inflamed site is cleared, our immune cells stop the production of inflammatory cells and start the production of anti-inflammatory cells.
When you’re in the inflammatory response stage, the signs and symptoms of inflammation are pain, redness, swelling, heat, and loss of function or limited range of movements.
The treatment should reduce the pain and swelling and prevent chronic inflammation. Resting the affected area is also essential, but keep the rest of your body active.
Repair and Regeneration Stage
During this stage, your body creates more collagen to create new tissue. A scar may also start to form.
At first, the forming tissues have weak spots, and collagen fibers are not organized, so when you move forcefully, you can disrupt the new tissue. This is why wounds open and bleed when you exert yourself too much. But eventually, the new tissues become tougher.
The signs and symptoms lessen during this stage. However, the pain remains, especially if the new tissue is stretched. There’s also some swelling and tenderness, so it’s still painful to touch your injury.
To promote tissue formation and facilitate recovery, focus on regaining the normal range of motion of the injured site.
Remodeling and Maturation Stage
At this point, the collagen fibers become more properly laid down, and the tissue continues to strengthen. As a result, your strength and range of motion also improve.
What are the types of inflammation?
There are two types of inflammation: acute and chronic.
Acute inflammation is short-lived, lasting for a few hours to a few days. For example, when you cut your finger while chopping onions, the pain, redness, swelling, heat, and loss of function (the five signs of acute inflammation) only happen for a short time before they subside.
After a couple of days or so, a scab forms over the wound, indicating it’s healing. Then, your injured finger stops hurting, and it can help you chop onions again.
On the other hand, chronic inflammation lasts several months, years, or even a lifetime.
Some of the reasons why chronic inflammation happens are:
-
the injury or damage is severe or widespread
-
the body takes time to remove the infection or repair the damaged tissues
-
prolonged exposure to low levels of irritants (e.g., when you are constantly exposed to toxins, such as industrial chemicals, for a long time)
-
acute inflammation happens repeatedly or doesn’t stop after the harmful stimuli are addressed
-
Autoimmune disease, a condition in which your immune system attacks normal, perfectly healthy, undamaged cells. Examples of autoimmune diseases are lupus and rheumatoid arthritis.
In these cases, your immune system is always active and vigilant, causing persistent inflammatory responses (e.g., the pain you may be feeling in your joints now and then).
For example, in the case of rheumatoid arthritis, WBCs seep inside your joints, causing them to swell and get irritated. WBCs can also destroy your cartilage, the cushion between your bones, which causes pain.
Impacts of chronic inflammation on health and aging

Chronic inflammation causes your immune cells and the chemicals they produce to build up, attack perfectly healthy cells and tissues, and cause serious diseases. In other words, your immune system turns against you.
Chronic inflammation leads to diseases that significantly threaten our health. Aside from autoimmune disease, chronic inflammation can also lead to diabetes, arthritis and joint disease, allergies, cardiovascular diseases, and Chronic Obstructive Pulmonary Disease (COPD).
In addition, chronic inflammation accelerates aging.
Chronic inflammation limits your movements, making you lose muscle mass and your ability to recover faster from injury, which further prolongs the inflammation. It’s a vicious cycle that leaves you sedentary and frail over the years.
Also, inflammation breaks down collagen, the most abundant protein in the body that gives structure and support to your tissue and organs. It’s what keeps your skin smooth, supple, and elastic.
Without enough collagen, signs of aging become visible such as wrinkles, crepey skin, and saggy skin.
How to reduce inflammation in the body?
Now that you know how dangerous chronic inflammation can be, let’s discuss how you can prevent it by reducing the inflammation in your body.
1. Eat anti-inflammatory foods
Although there are many anti-inflammatory drugs to choose from, reducing inflammation naturally by eating anti-inflammatory foods is a better option because of their lack of toxins and side effects.
Some of the best anti-inflammatory foods are berries, grapes, pomegranate, cherries, beets, cruciferous vegetables, mushrooms, ginger, turmeric, and green tea.
These anti-inflammatory fruits, vegetables, and herbs are rich in antioxidants and anti-inflammatory agents that fight oxidative stress, maintain your health, and restore your youthful glow.
You can incorporate these anti-inflammatory foods into your diet and reap their benefits by taking a whole-food-based superfood greens powder like AgelessLX Power Greens.
AgelessLX Power Greens is an all-in-one nutrition solution made from REAL, whole foods. Aside from anti-inflammatory agents, it also contains a blend of prebiotics, probiotics, and digestive enzymes that eliminate bloating and improve gut health.
Additionally, it’s packed with adaptogens proven to control rage-inducing, tear-jerking mood swings.
AgelessLX Power Greens provides all the nutrients you can get from 6 servings of veggies and more, making it the perfect nutritional insurance for busy women like you. Plus, it’s yummy and only has 30 calories, so you can enjoy it guilt-free.
2. Maintain a healthy weight.
Being overweight makes you vulnerable to many diseases like diabetes and heart diseases. But little did you know that excess fat also puts you at risk of chronic inflammation.
According to research, visceral fat— those hidden deep in the belly area and around your organs— secretes enormous amounts of cytokines that promote inflammation.
So, avoid the accumulation of visceral fat by eating smart. Avoid eating refined sugar and saturated fat. Instead, load up on leafy greens, yogurt, cheese, and milk.
Also, take in more calcium and vitamin D; they’re associated with less visceral fat.

3. Exercise.
Exercise helps you drop off excess fat from your body, including visceral fat, which may lead to inflammation. You can do 10 minutes of extreme workout or 30 minutes of moderate exercise.
High-Intensity Interval Training (HIIT), weight lifting, bodyweight exercises, resistance training, and practicing yoga are excellent options.
In addition, exercise soothes inflammation by increasing blood flow, oxygen, and nutrients to inflamed areas of your body, which speeds up tissue repair.
Exercise also improves muscle mass and strength, enhancing its ability to recover quickly from damage and injury.

4. Get enough deep sleep.
It’s essential to sleep for 7 to 9 hours every night, but getting enough deep sleep matters even more.
Sleep has different stages, and it’s only in deep sleep that our body undergoes repair, restoration, and rejuvenation. Without it, we won’t feel refreshed and well-rested the following.
During deep sleep, our body takes out the trash (the metabolic waste accumulated throughout the day), increases blood flow to your muscles, repairs damaged tissues, regenerates cells, and reduces inflammation.
Essentially, deep sleep amplifies the health benefits of eating healthy and exercising.
Did you find this article helpful? Share it on social to help others understand and reduce inflammation.
LINKS:
-
Acute Inflammatory Response - StatPearls - NCBI Bookshelf (nih.gov)
-
Chronic Inflammation - StatPearls - NCBI Bookshelf (nih.gov)
-
What Are Common Symptoms of Autoimmune Disease? | Johns Hopkins Medicine
-
Definition of immune cell - NCI Dictionary of Cancer Terms - National Cancer Institute
-
Definition of white blood cell - NCI Dictionary of Cancer Terms - National Cancer Institute
-
Definition of cytokine - NCI Dictionary of Cancer Terms - National Cancer Institute
-
Q&A: What are pathogens, and what have they done to and for us? - PMC (nih.gov)
-
Definition of reactive oxygen species - NCI Dictionary of Cancer Terms - National Cancer Institute
-
Oxidative Stress: Harms and Benefits for Human Health - PMC (nih.gov)
-
Fight Inflammation to Help Prevent Heart Disease | Johns Hopkins Medicine
-
Visceral Fat: Why It’s Dangerous and How to Lose It (webmd.com)
*These statements have not been evaluated by the Food and Drug Administration. These products are not intended to diagnose, treat, cure, or prevent any disease.
**Individuals may have received free product or compensation in exchange for their honest review. Individual results will vary. All other benefits/effects noted in these testimonials/reviews are the individuals’ personal opinions and have not been studied.
© 2024 AgelessLX ®️. All rights reserved.